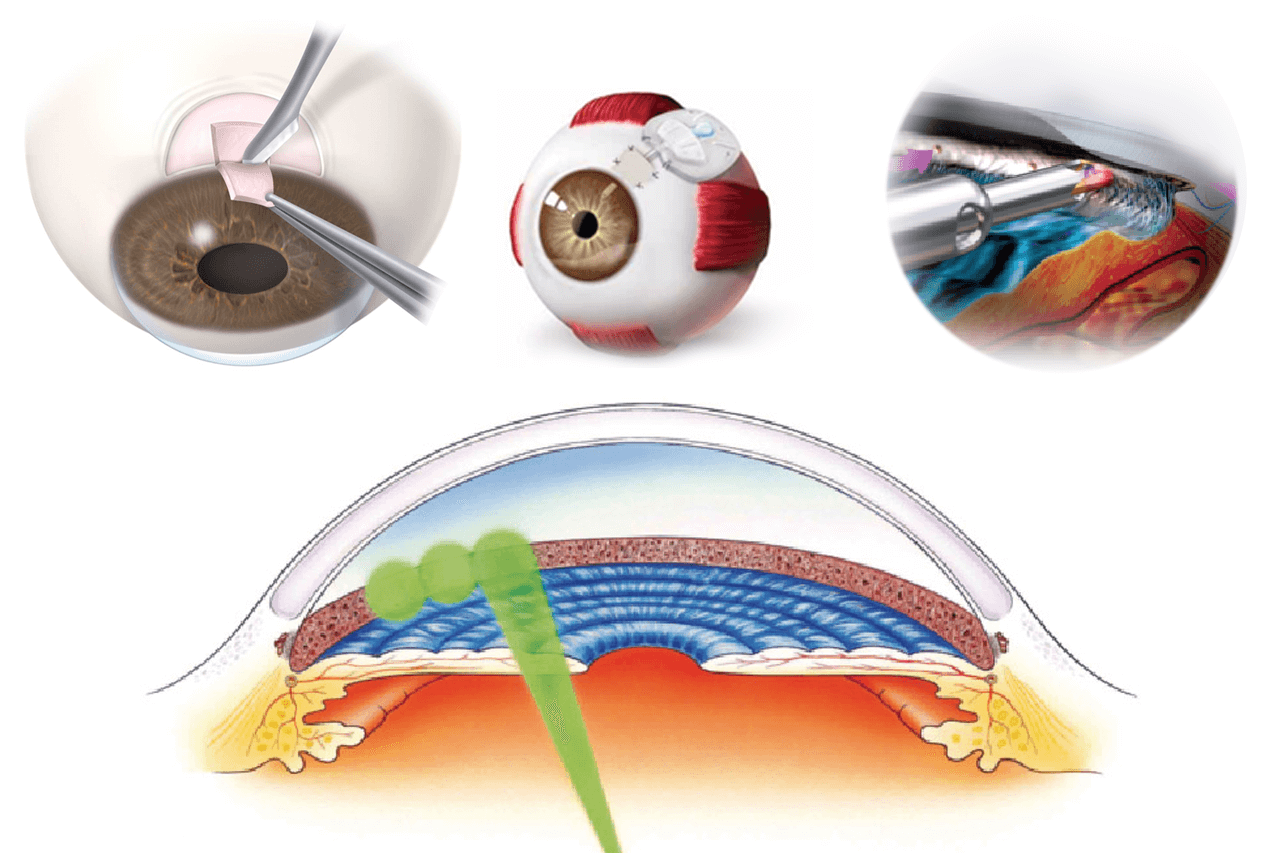
Selective Laser Trabeculoplasty
Now, a Gentler Glaucoma Laser Surgery
for open angle glaucoma • alternative to eye drop • no thermal damage • 5-10 minute treatment • non-invasive
What Is Selective Laser Trabeculoplasty
Selective Laser Trabeculoplasty (SLT) is a type of laser surgery that is used to lower intraocular pressure in glaucoma. In most open-angle glaucomas the aqueous fluid is unable to pass through the Trabecular Meshwork (drainage grate inside the eye) as easily as it should.[1]
Partly due to this knowledge, most surgical treatments of glaucoma have focused on improving passage of fluid across this meshwork or simply bypassing the meshwork altogether. Laser trabeculoplasty improves flow of fluid across the trabecular meshwork by focusing wavelengths of light onto the trabecular meshwork. Essentially, 50-100+ very short laser pulses are used to gently irradiate the trabecular meshwork. No holes are created, but for reasons that are not entirely understood, this allows fluid to more easily leave the eye.[2]
How Long Has Selective Laser Trabeculoplasty (SLT) Been Around?
The concept of using light energy to open up the trabecular meshwork dates back to 1961.[3] However, It was not until 1979 that Laser Trabeculoplasty (LT) was introduced for the treatment of glaucoma.[4] Selective Laser Trabeculoplasty (SLT) was first reported in 1995.[5] and had gained FDA approval in March 2001 (according to US reimbursement codes data). To date, It is rapidly becoming the preferred method of laser surgery for treating primary open angle glaucoma. It can also be performed on patients who have already had received a full treatment of ALT.[6]
How Is SLT Performed?
SLT uses a “Q-switched, frequency-doubled Nd:YAG laser”. This laser energy is preferentially absorbed by the pigment-containing cells in the trabecular meshwork while cells without pigment are left undamaged. Because SLT does not “coagulate” (or melt) tissue this results in a less traumatic laser treatment compared to ALT.[7]
What Are The Risks And Side Effects Of SLT?
Laser Trabeculoplasty is usually painless (though not always), fast, and relatively safe. As such, it can be offered to almost anyone with open angle glaucoma at almost any stage in the disease. As with all surgical procedures, however, there are risks associated with Laser Trabeculoplasty such as 1) Intraocular Elevation (Spike); however, these elevations in IOP are generally short-lived, 2) Scarring of the Eye’s Drainage System (Peripheral Anterior Synechiae) is seen in less than 3% of eyes treated with Selective Laser Trabeculoplasty (SLT).[8] and rarely encountered additional risks of Laser Trabeculoplasty include corneal damage and swelling of the central retina (macula), both of which could result in loss of vision.
How Effective Is Selective Laser Trabeculoplasty?
Laser Trabeculoplasty has a long track record of effectively lowering the IOP while presenting relatively low risk to those receiving this treatment. It’s success is dependent upon how much of the trabecular meshwork is treated. When only half of the trabecular meshwork is treated (180 degrees) SLT successfully lowers the intraocular pressure (IOP) 65% of the time with an average reduction in IOP of just over 4mmHg (range of 2 to 18mmHg).[10] However, when a full 360 degree treatment is applied the IOP can be expected to be reduced in almost all eyes by 11-40%.[11]
Laser Trabeculoplasty works about as well as a single glaucoma drop. Given the long-term side effects associated with chronic glaucoma drop use as well as the cost of medications most patients with open angle glaucoma should at least consider the option of SLT.
Why Choose Selective Laser Trabeculoplasty (SLT) ?
SLT Can Be Repeated
Selective Laser Trabeculoplasty (SLT) may be repeated multiple times so long as there is an initial IOP-lowering response to the first treatment.[13] When SLT is repeated after the first SLT treatment has worn off the IOP may be further reduced by about 20% in 43-67% of treated eyes.[14] Eventually, however, re-treatments lose their effect at which time medical or non-laser surgical options must be considered if the IOP is too high.
SLT does not limit future treatment options
Selective Laser Trabeculoplasty (SLT) is less likely to limit future glaucoma surgical options such as the expanding number of available minimally invasive glaucoma surgeries (MIGS). The laser does not affect the success of other types of treatment, such as Canaloplasty.
Who Is a Candidate For Selective Laser Trabeculoplasty?
Most anyone with open angle glaucoma that requires treatment is a candidate for Laser Trabeculoplasty. Although it is generally offered to patients in the USA after drops have been tried (and failed), there is some evidence to suggest that laser trabeculoplasty may work better if it is done prior to drop use. Indeed, multiple studies support the use of laser trabeculoplasty as a reasonable first choice in the treatment of glaucoma.[15]
- You have open angle glaucoma, pseudoexfoliation or pigmentary glaucoma
- Drops aren’t working for you
- You can’t keep up with Drops Regimen – a hassle and/or too costly
- You have not had multiple prior glaucoma operations
- Pre-treatment IOP not higher than 30mmHg
What Top Glaucoma Surgeons Are Saying
Selective laser trabeculoplasty is becoming more commonly recommended primarily because it doesn’t destroy tissue. It can be performed on its own or even after ALT. It’s less traumatic because it doesn’t coagulate tissue (less damage), it’s quick and it’s usually painless.
One key aspect of SLT is a favorable side effect profile, even when compared with glaucoma medications. Post-operative inflammation is common but generally mild, and treated with observation or eye drops or an oral non-steroidal anti-inflammatory drug.[9]
SLT causes really no thermal damage to the adjacent cells or structures compared to MLT or ALT. As thermal damage is not occurring, the Schlemm’s canal is not fused together, the process can theoretically be repeated in the same eye.
I think the consensus is that, when you’re looking at laser trabeculoplasty as an initial therapy, it seems to be a winner on cost-effectiveness.

LATEST ARTICLES ON DR. RICHARDSON’S GLAUCOMA HEALTHHUB
References
1) Grant WM. Further studies on facility of flow through the trabecular meshwork. AMA Arch Ophthalmol. 1958;60(4 Part 1):523-33.
Grant WM. Experimental aqueous perfusion in enucleated human eyes. Arch Ophthalmol. 1963;69:783-801.
2) Pohjanpelto P. Argon laser treatment of the anterior chamber angle for increased intraocular pressure. Acta Ophthalmol. 1981;59(2):211-220.
Lichter PR. Argon laser trabeculoplasty. Trans Am Ophthalmol Soc. 1982;80:288-301.
Brubaker RF, Liesegang TJ. Effect of trabecular photocoagulation on the aqueous humor dynamics of the human eye. Am J Ophthalmol. 1983;96(2):139-147.
3) Zweng HC, flocks M. Experimental photocoagulation of the anterior chamber angle. A preliminary report. Am J Ophthalmol. 1961;52:163-165.
4) Wise JB, Witter SL. Argon laser therapy for open-angle glaucoma. A pilot study. Arch Ophthalmol. 1979;97(2):319-322.
5) Latina MA, Park C. Selective targeting of trabecular meshwork cells: in vitro studi es of pulsed and CW la ser interactions. Exp Eye Res. 1995; 60:359-71.
6) Damji KF, Shah KC, Rock WJ, et al. Selective laser trabeculoplasty v argon laser trabeculoplasty: a prospective randomised clinical trial. Br J Ophthalmol. 1999;83(6):718-722.
7) KramerTR, Noecker RJ. Comparison of the morphologic changes after selective laser trabeculoplasty and argon laser trabeculoplasty in human eye bank eyes. Ophthalmology. 2001;108:773-9.
8) Wong MOM, Lee JWY, Choy BNK, et al. Systematic review and meta-analysis on the efficacy of selective laser trabeculoplasty in o pen-angle glaucoma. Surv Ophthalmol. 2014[Published online].
9) Selective Laser Trabeculoplasty: 10 Commonly Asked Questions. http://www.glaucoma.org/treatment/selective-laser-trabeculoplasty-10-commonly-asked-questions.php
10) Kajiya S, Hayakawa K, Sawaguchi S. Clinical results of selective laser trabeculoplasty. Jpn J Ophthalmol. 2000;44(5):574-575
11) Lanzetta P, Menchini U, Virgili G. Immediate intraocular pressure response to selective laser trabeculoplasty. Br J Ophthalmol. 1999;83(1):29-32.
Stein JD, Challa P. Mechanisms of action and efficacy of argon laser trabeculoplasty and selective laser trabeculoplasty. Curr Opin Ophthalmol. 2007;18:140-5.
12) A Decade of Selective Laser Trabeculoplasty . http://ophthalmologytimes.modernmedicine.com/sites/default/files/images/OphthalmologyTimesEurope/PDF/A-Decade-of-Selective-Lase-Trabeculoplasty.pdf
13) Hong BK, Winer JC, Martone JF, et al. Repeat selective laser trabeculoplasty. J Glaucoma. 2009;18(3):180-183.
14) Avery N, Ang GS, Nicholas S, et al. Repeatability of primary selective laser trabeculoplasty in patients with primary open-angle glaucoma. Int Ophthalmol. 2013;33:501-6.
Hong BK, Winer JC, Martone JF, et al. Repeat selective laser trabeculoplasty. J Glaucoma. 2009;18:180-3.
15) Rosenthal AR, Chaudhuri PR, Chiapella AP. Laser trabeculoplasty primary therapy in open-angle glaucoma. A preliminary report. Arch Ophthalmol. 1984;102(5):699-701.
Thomas JV, El-Mofty A, Hamdy EE, et al. Argon laser trabeculoplasty as initial therapy for glaucoma. Arch Ophthalmol. 1984;102(5):702-703.
Migdal C, Hitching R. Primary therapy for chronic simple glaucoma the role of argon laser trabeculoplasty. Trans Ophthalmol Soc UK. 1985;104(1):62-66.
Sherwood MB, Lattimer J, Hitching RA. Laser trabeculoplasty as supplementary treatment for primary open angle glaucoma. Br J Ophthalmol. 1987;71(3):188-191.
Tuulonen A, Koponen J, Alanko HI, et al. Laser trabeculoplasty versus medication treatment as primary therapy for glaucoma. Acta Ophthalmol. 1989;67(3):275-280.
The Glaucoma Laser Trial Research Group. The Glaucoma Laser Trial (GLT). 2. Results of argon laser trabeculoplasty versus topical medications. Ophthalmology. 1990;97(11):1403-1413.
Elsas T, Johnsen H. Long-term efficacy of primary laser trabeculoplasty. Br J Ophthalmol. 1991;75(1):34-37.
The Glaucoma Laser Trial Research Group. The Glaucoma Laser Trial (GLT) and glaucoma laser trial follow-up study: 7. Results. Am J Ophthalmol. 1995;120(6):718-731.
Contact Us to See If SLT Is for You
Dr. David Richardson offers Selective Laser Trabeculoplasty (SLT) as an outpatient procedure in his San Marino Eye office. SLT can be performed on the same day as most examinations and the whole procedure takes 10 minutes or less. SLT is a gentler glaucoma laser surgery. Contact Dr. David Richardson immediately to see if SLT is for you.
Call today to schedule an appointment with Dr. Richardson at
(626) 289 7856